
Introduction
Healthcare organizations face mounting pressure to improve patient safety while managing regulatory requirements from HIPAA, Joint Commission, and CMS. Yet incident reporting systems often capture only 14% of actual patient harm events, leaving hospitals blind to 86% of safety issues.
This gap creates preventable patient harm that costs the U.S. healthcare system billions annually while putting patients at unnecessary risk.
Incident reporting delivers real value through reduced errors, faster response times, and measurable improvements in patient outcomes. Modern incident management software transforms scattered safety data into actionable intelligence that prevents harm and positions organizations ahead of regulatory expectations.
TLDR
- Centralizes incident reporting and transforms scattered data into actionable safety insights
- Reduces administrative burden by 60-84% and accelerates resolution by 67%
- Increases reporting rates by 300-400% through user-friendly, anonymous reporting
- Delivers real-time alerts, compliance tracking, trend analytics, and EHR/QMS integration
- Prevents repeat events and generates cost savings through proactive pattern identification
What Is Healthcare Incident Management Software
Healthcare incident management software is a digital platform that enables staff to report, track, investigate, and analyze adverse events, near misses, and safety concerns in real-time from any device.
Healthcare systems use these platforms across hospitals, clinics, long-term care facilities, and emergency departments to manage patient safety events, workplace injuries, equipment failures, medication errors, and compliance incidents.
These platforms go beyond simple documentation to deliver measurable safety improvements:
- Identify patterns across incidents to prevent recurrence
- Meet regulatory requirements with audit-ready reporting
- Protect patients through faster incident response
- Reduce organizational risk and associated costs
- Transform reactive documentation into proactive safety management
Modern systems create the visibility and accountability healthcare organizations need to deliver consistently safe patient care.
7 Critical Benefits of Incident Management Software in Healthcare
The seven benefits below focus on measurable, operational impact rather than theoretical advantages. Each benefit is tied to outcomes healthcare organizations track: patient safety metrics, compliance scores, staff efficiency, cost avoidance, and quality indicators.
These advantages are drawn from real-world implementations across hospitals and healthcare systems, supported by data showing concrete improvements in safety, efficiency, and financial performance.
Benefit 1: Real-Time Incident Reporting and Response
What this means: Staff can report incidents immediately via mobile devices, web portals, or dedicated hotlines with 24/7 access, eliminating delays associated with paper forms or waiting for computers.
Automated alerts notify relevant personnel instantly, incident details are captured with timestamps and location data, and routing rules ensure the right people respond immediately based on incident type and severity.
How software creates this advantage: Integrated electronic systems allow staff to report incidents without the "extra time and effort" required by paper forms or separate logins.
Digital platforms facilitate immediate response to reduce the consequences of incidents, while manual systems often delay recognition and intervention.
Why this matters: Structured record reviews detect 19.9 preventable adverse events per 1,000 patient-days versus only 3.4 via traditional incident reporting systems. This detection gap directly impacts patient outcomes.
Faster reporting means quicker intervention to address ongoing safety issues, prevents incident details from being forgotten or diluted, and enables immediate corrective action that can prevent harm escalation.
KPIs impacted:
- Incident response time
- Time from occurrence to documentation
- Time to resolution
- Patient safety event escalation rates
- Staff response efficiency

When this advantage matters most:
- High-acuity environments (emergency departments, ICUs, surgical units)
- Off-hours when administrative staff are unavailable
- Multi-site healthcare systems where coordination is challenging
- Time-sensitive safety issues like medication errors or patient falls
Benefit 2: Comprehensive Trend Analysis and Pattern Recognition
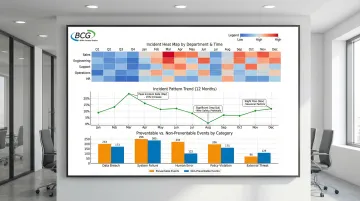
What this means: Software automatically combines incident data across departments, shifts, and timeframes, using analytics dashboards to surface recurring issues, high-risk areas, and emerging patterns that would be invisible in manual systems.
Centralized databases allow filtering by incident type, location, severity, staff involved, time of day, and patient demographics.
How software creates this advantage: Visual analytics tools—heat maps, trend graphs, comparison charts—make patterns immediately visible to quality teams and leadership.
Electronic systems allow risk managers to "view incidents as soon as they occur and analyze the reports to identify any existing trends," enabling proactive prevention rather than reactive response.
Why this matters: A documented case study shows needlestick injuries dropping from 11 in 2018 to 2 in 2021 after implementing root cause analysis via an electronic system. Pattern recognition enables targeted interventions before more incidents occur.
Research confirms that 43% of harm events are preventable when patterns are identified early.
KPIs impacted:
- Repeat incident rates
- Incidents by department/unit
- Incidents by type over time
- Preventable adverse events
- Quality improvement initiative success rates
- HCAHPS safety scores
When this advantage matters most:
- Quality improvement initiatives requiring baseline data
- Preparing for Joint Commission or CMS surveys
- Multi-facility organizations needing comparative analysis
- Demonstrating continuous improvement to regulatory bodies
Benefit 3: Enhanced Regulatory Compliance and Audit Readiness
What this means: Software maintains complete audit trails with timestamps, user actions, investigation notes, and corrective actions. All documentation is automatically organized and accessible for regulatory inspections, accreditation surveys, and internal audits.
Built-in compliance frameworks align with HIPAA, Joint Commission standards, CMS Conditions of Participation, and state reporting requirements.
How software creates this advantage: Automated workflows ensure mandatory reporting timelines are met, and privileged investigation features protect sensitive peer review materials.
The Joint Commission requires organizations to share root cause analyses and action plans for sentinel events—digital platforms standardize this submission process.
Why this matters: 22% of hospitals participating in the HAC program were penalized, and a recent OIG report found hospitals failed to report 67% of captured harm events that required external reporting.
Manual systems create compliance gaps through lost paperwork, missed reporting deadlines, incomplete investigations, and inability to demonstrate systematic response to incidents. Automated systems eliminate these risks while reducing audit preparation time by 70-80%.
KPIs impacted:
- Regulatory citation rates
- Audit preparation time
- Mandatory reporting compliance rates
- Documentation completeness scores
- Time to generate compliance reports
- Deficiency correction tracking

When this advantage matters most:
- Joint Commission surveys, CMS audits, or state health department inspections
- Organizations facing increased regulatory scrutiny
- Facilities with previous compliance issues requiring remediation
- Managing reportable events that require external notification
Benefit 4: Increased Reporting Through User-Friendly Interfaces
What this means: Modern incident management platforms offer intuitive mobile apps, simple web forms, QR code access, and anonymous reporting options that remove barriers preventing staff from documenting incidents.
Pre-populated dropdown menus reduce typing, smart forms adapt based on incident type, mobile access allows reporting at point of occurrence, and quick submission (2-3 minutes) fits into busy clinical workflows without disrupting patient care.
How software creates this advantage: Integrated systems achieved 85.1% reporting compliance because the process was embedded in workflow, compared to typical rates of 4.3% to 23% for non-integrated systems.
Anonymous options eliminate fear of retaliation. Mobile access means staff can report immediately rather than waiting to find a computer or paper form.
Why this matters: Studies show only 10-20% of incidents get documented with manual systems, meaning organizations are blind to 80-90% of safety issues. Research indicates nurses may underreport medical errors by 50% to 96%.
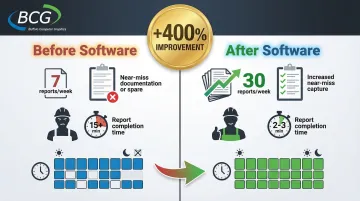
One documented implementation saw reporting increase from 7 incidents/week to 30 incidents/week—a 4x increase. This gives leadership complete visibility into the actual safety landscape rather than just the most severe events.
KPIs impacted:
- Incident reporting rates
- Near-miss reporting frequency
- Staff participation in safety reporting
- Time to complete incident report
- Reporting rates by shift/department
- Anonymous vs. identified reports ratio
When this advantage matters most:
- Organizations with historically low reporting rates
- Establishing a "just culture" safety environment
- Busy clinical areas where staff time is extremely limited
- Addressing underreporting during specific shifts (nights/weekends)
- Leadership seeking visibility beyond severe events
Benefit 5: Significant Cost Reduction Through Prevention and Efficiency
What this means: Incident management software reduces costs through multiple mechanisms:
- Preventing repeat incidents saves millions in adverse event costs
- Automation eliminates administrative labor
- Faster resolution minimizes operational disruptions
- Early intervention prevents minor issues from becoming expensive crises
How software creates this advantage:
- Analytics identify high-cost incident patterns allowing targeted prevention
- Automated workflows eliminate manual tracking/follow-up labor (saving 15-30 hours per month)
- Faster incident resolution prevents extended length of stay and readmissions
- Proactive risk identification avoids costly sentinel events and litigation
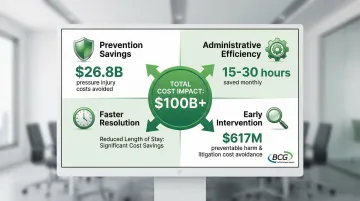
Why this matters: Hospital-acquired pressure injuries alone could cost the U.S. over $26.8 billion, while preventable harm events in Massachusetts resulted in over $617 million in excess claims. Even small improvements in prevention generate massive savings.
A documented quality improvement initiative led to a 77% reduction in pressure injuries, while administrative automation allows reallocation of staff to direct patient care rather than paperwork.
KPIs impacted:
- Cost per adverse event
- Preventable adverse event rates
- Administrative labor hours
- Incident-related length of stay
- Readmission rates
- Litigation and settlement costs
- Staff productivity metrics
- Revenue impact from operational disruptions
When this advantage matters most:
- Organizations facing financial pressures or narrow margins
- High-frequency incident types that accumulate significant costs
- Facilities with high administrative burden diverting resources from patient care
- Demonstrating ROI to leadership or board
- Competitive markets where operational efficiency impacts financial viability
Benefit 6: Improved Staff Engagement and Safety Culture
What this means: When staff see that reporting incidents leads to actual improvements rather than punishment, they become active participants in safety. Modern systems include feedback loops, action tracking, and visible outcomes that demonstrate leadership commitment to addressing concerns.
How software creates this advantage: Anonymous reporting eliminates fear, automated acknowledgment confirms reports were received, transparent investigation tracking shows progress, staff can see what actions resulted from their reports, and closed-loop communication demonstrates that leadership values frontline input and takes safety seriously.
Why this matters: A positive safety culture is associated with fewer hospital-based adverse events, and strong safety cultures correlate with improved patient satisfaction.
Organizations with strong safety cultures where staff feel empowered to report have 50-70% fewer serious safety events. Engaged staff become the eyes and ears of quality improvement, catching issues before they harm patients, while disengaged staff in punitive cultures hide problems until they become crises.
KPIs impacted:
- Safety culture survey scores
- Staff participation rates in safety reporting
- Anonymous vs. identified reporting ratios
- Staff satisfaction with safety processes
- Time from report to feedback
- Staff turnover in high-risk units
- Near-miss to adverse event ratios
When this advantage matters most:
- Organizations shifting from blame culture to just culture
- Units with high staff turnover or low morale
- Leadership engaging frontline staff in quality improvement
- Increasing near-miss reporting that provides early warning of systemic issues
Benefit 7: Seamless Integration with Existing Healthcare Systems
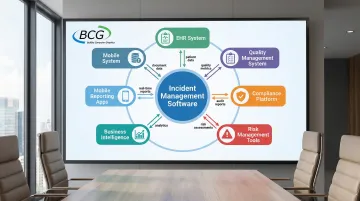
What this means: Modern incident management software connects with Electronic Health Records (EHR), Quality Management Systems (QMS), compliance platforms, risk management tools, and business intelligence systems—eliminating data silos and enabling comprehensive safety oversight without duplicate data entry.
How software creates this advantage: API connections and HL7 interfaces allow two-way data flow. Incidents can be linked to patient records for complete context, integration with QMS enables correlation of incidents with quality metrics, and consolidated dashboards provide single-source visibility across all safety and quality data streams.
Why this matters: Fragmented systems force staff to enter the same information multiple times, create inconsistencies between databases, prevent comprehensive analysis of relationships between incidents and outcomes, and waste valuable time on manual data reconciliation.
Integration enables real-time data analytics that allow providers to identify risks proactively rather than reactively, while eliminating the inefficiencies that plague siloed systems.
KPIs impacted:
- Data entry time
- Data accuracy and consistency rates
- Time to generate cross-system reports
- Analytics sophistication level
- Staff time spent on manual data reconciliation
- Completeness of incident context
- Ability to correlate incidents with patient outcomes
When this advantage matters most:
- Large healthcare systems with multiple existing platforms
- Organizations needing comprehensive views of safety across quality domains
- System implementations or upgrades
- Advanced analytics requiring data from multiple sources
What Happens Without Proper Incident Management Systems
Organizations relying on manual or inadequate systems face serious consequences. According to research from AHRQ's Patient Safety Network, 86% of patient harm events go unreported, leaving organizations blind to actual safety risks. Patterns remain invisible until sentinel events occur, and delayed responses allow minor issues to escalate into serious harm.
This reporting gap creates cascading operational problems:
- Manual tracking consumes 20-30 hours monthly of administrative time that could be spent on patient care
- Compliance gaps create regulatory citation risks—the OIG explicitly stated that when hospitals fail to capture harm events, they "stymie independent feedback needed to take corrective actions"
- Organizations face potential penalties, with 22% of hospitals in the HAC program receiving financial penalties
The financial impact is substantial. Preventable adverse events cost billions annually across healthcare, with pressure injuries alone representing over $26 billion in potential costs.
Organizations without trend data waste resources addressing symptoms rather than root causes. Staff frustration with cumbersome reporting reduces engagement in safety initiatives and contributes to burnout.
How to Maximize Value from Incident Management Software
Build a Culture of Reporting
Drive user adoption through comprehensive training, mobile accessibility, and demonstrating quick wins where staff reports led to visible improvements. System value is directly tied to reporting completeness, so removing barriers and showing impact drives engagement.
Make reporting as easy as sending a text message, and ensure anonymous options eliminate fear of retaliation.
Once reporting becomes routine, establish regular review cycles where leadership analyzes trends monthly, shares findings with staff, and implements targeted interventions based on data patterns. Close the loop by communicating what actions resulted from reports. This approach demonstrates the system drives real change rather than creating a documentation black hole.
Integrate Advanced Capabilities
Leverage advanced features including:
- Custom workflows for your specific incident types
- Integration with existing systems to eliminate duplicate entry
- Automated compliance reporting to reduce audit preparation burden
- Analytics dashboards for data-driven decision making
- Real-time alerts for high-severity incidents
- Mobile reporting for point-of-care documentation
For healthcare organizations managing emergency coordination alongside patient safety, platforms such as DisasterLAN by Buffalo Computer Graphics offer FEMA NIMS STEP compliance—the first and only incident management system evaluated as fully compliant with NIMS and ICS principles.
This ensures the system meets rigorous standards for emergency response coordination and interoperability with emergency management agencies during disasters or mass casualty events.
Conclusion
The value of incident management software lies in transforming scattered safety data into actionable intelligence that prevents harm, reduces costs, and demonstrates commitment to quality.
Benefits compound over time as reporting increases, patterns emerge, interventions grow more targeted, and safety culture strengthens.
Early adoption positions organizations ahead of regulatory expectations and competitive pressures. The patient safety and risk software market will reach $2.99 billion by 2030, driven by demand for real-time analytics and regulatory compliance.
Leading healthcare organizations treat incident management as a strategic investment in patient safety and operational excellence rather than a compliance checkbox, with measurable returns in reduced adverse events, improved outcomes, and enhanced reputation.
Frequently Asked Questions
What is the average ROI timeline for healthcare incident management software?
Most organizations see positive ROI within 6-12 months through administrative time savings and prevention of serious adverse events. Documented cases show 77% reductions in specific incident types and 15-30 hours saved monthly.
How does incident management software integrate with our existing EHR system?
Modern platforms use HL7 interfaces and APIs to connect with major EHR systems while maintaining HIPAA compliance. This eliminates duplicate data entry and enables correlation of incidents with patient outcomes.
What features should we prioritize when selecting incident management software?
Prioritize mobile accessibility, automated workflows and alerts, robust analytics, compliance frameworks, EHR integration, and anonymous reporting options. Quick reporting interfaces (under 3 minutes) drive adoption.
How do we encourage staff to actually use the incident reporting system?
Make reporting simple with anonymous options, demonstrate visible leadership response, and show staff what improvements resulted from their reports. Research shows reporting increases 300-400% when staff see their input drives real change.
What makes FEMA NIMS STEP compliant systems different for healthcare incident management?
FEMA NIMS STEP compliance ensures interoperability with emergency management agencies and structured incident command principles—critical for coordinating with external responders during disasters or mass casualty events. BCG's DLAN is the first and only incident management system to achieve this certification.
How does incident management software help with Joint Commission accreditation?
The software maintains complete audit trails, demonstrates systematic response to incidents, tracks corrective actions through completion, and generates reports showing continuous quality improvement—all key requirements for Joint Commission standards. Automated documentation eliminates gaps that lead to citations, while after-action reports provide the evidence surveyors need to verify compliance with emergency management and patient safety standards.


